Standard analysis of in vitro (culture-adapted Plasmodium strains) and ex vivo (fresh Plasmodium clinical isolates) assay data is commonly conducted by using non-linear regression to fit a sigmoid E max model to each sample’s concentration-effect data. Although these assays are highly informative, the comparison of data between laboratories or field sites is often problematic as numerous variations exist between protocols, such as the initial parasitaemia, incubation time, culture haematocrit, and the use of alternative media and supplements. In most, the parasites’ drug susceptibility is defined by measuring growth (i.e., schizont maturation) or replication (i.e., re-invasion assays) in the presence of varying concentrations of anti-malarial compounds. Ī variety of assays are available to measure drug susceptibility in Plasmodium falciparum. In addition, in vitro assays enable the measurement of drug sensitivity without the confounding effects of clinical efficacy such as host immunity and the pharmacokinetics of the drug. In vitro assays also provide an opportunity to assess drug susceptibility of parasites to individual drugs, thereby allowing preventive measures to be taken before clinical treatment failure occurs. Although artemisinin-based combination therapy (ACT) has been implemented widely for the treatment of falciparum malaria and has proven to be beneficial, it is important to consider that resistance to one component of the therapy can be masked by a partner drug which retains high anti-malarial efficacy.

In vitro assays for assessing anti-malarial drug susceptibility are an important part of monitoring drug resistance and investigation of novel anti-malarial compounds. Resistance has emerged and spread to all currently available anti-malarials and reinforces the need for better surveillance strategies. Efforts to control and eliminate malaria have failed repeatedly, often due to the spread of drug-resistant parasites and vectors. Malaria remains a serious public health problem in endemic countries. In view of processing time and ease of analysis, GraphPad Prism 6.0 or IVART are best suited for routine and large-scale drug susceptibility testing. IC 50 estimates obtained from the programs tested were comparable.
GRAPHPAD PRISM 6 PRICE OFFLINE
Data analysis using WinNonlin or ICE took the longest computationally, whilst the offline ability of GraphPad Prism 6.0 to analyse multiple isolates and drugs simultaneously made it the fastest among the programs tested. WinNonlin, GraphPad Prism 6.0, IVART, and ICE provide alerts for non-fitting data and incorrect data entry, facilitating data interpretation. While HN-NonLin and IVART allow users to enter the data in 96-well format, IVART and GraphPad Prism 6.0 are capable to analyse multiple isolates and drugs in parallel. The user-friendliness varied between packages. There was good correlation of results derived from alternative statistical programs and non-linear mixed-effects modelling (NONMEM) which models all isolate data simultaneously.

The IC 50 and slope estimates were similar across all statistical packages for all drugs tested in both species. vivax clinical isolates tested with five anti-malarial agents: chloroquine, amodiaquine, piperaquine, mefloquine, and artesunate. In this study, licensed computer programs WinNonlin and GraphPad Prism 6.0, and the open access programs HN-NonLin, Antimalarial ICEstimator (ICE), and In Vitro Analysis and Reporting Tool (IVART) were tested for their ease of use and ability to estimate reliable IC 50 values from raw drug response data from 31 Plasmodium falciparum and 29 P.
The half-maximal inhibition of growth (IC 50) is the most commonly reported parameter expressing drug susceptibility, derived by a variety of statistical approaches, each with its own advantages and disadvantages.
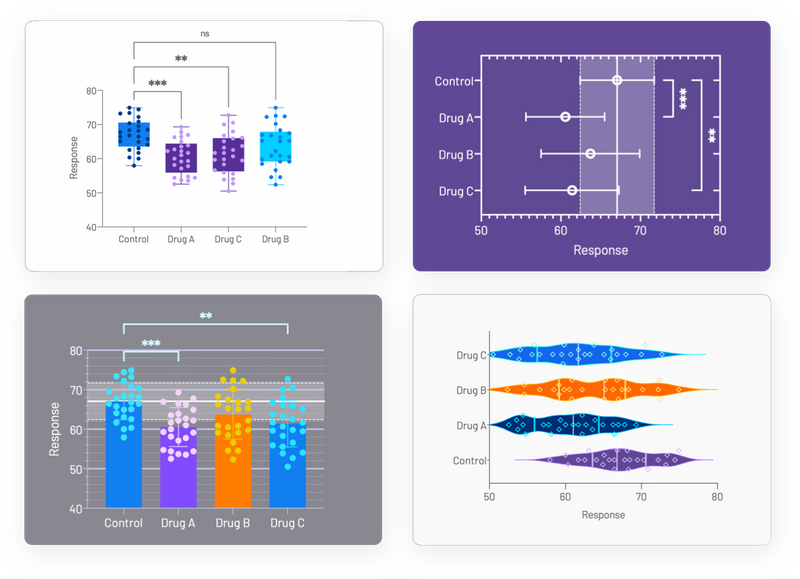
In vitro drug susceptibility testing of malaria parasites remains an important component of surveillance for anti-malarial drug resistance.
